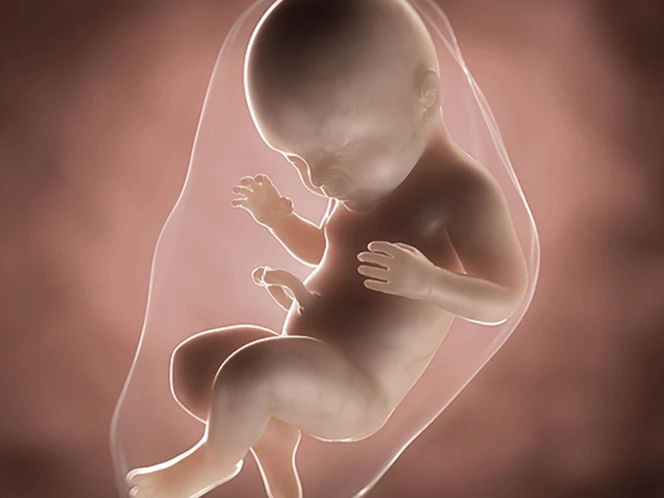
Most of the weight gain you’re likely to experience during pregnancy happens after week 20 as your baby, uterus, and placenta grow. Your body also stores fat to help you produce breast milk once your baby is born4.
As you begin your third trimester, carrying this extra weight can be tiring. Your growing baby might also be putting pressure on your back and organs, leading to symptoms like backache and indigestion1. Listen to your body and rest whenever you get the opportunity.
Our expert midwife also advises that you may experience another hormonal shift at this point in your pregnancy, similar to that you may have noticed during your first trimester, so keep an eye on how you’re feeling both physically and mentally.
In addition, from 28 weeks, your midwife will start to pay closer attention to your growing baby bump, and measure it with a tape measure. This is so they can monitor your baby’s Symphysis Fundal Height (SFH) and record the measurements on a perosnalised growth chart. If your midwife has any concerns, they may organise for you to have a growth scan, to ensure that your baby is growing as they should5, 6.