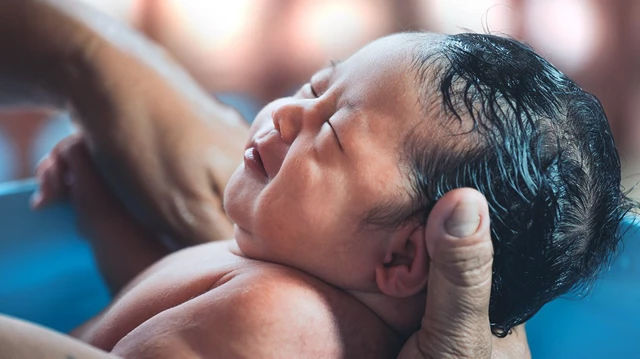
Most caesareans are performed under regional anaesthetic to numb you from the waist down, using either an epidural or a spinal block6. This means you’re awake as your baby is born, so that you can start bonding at the earliest opportunity.
You’ll normally have a screen put up across your chest so that you can’t see the operation itself6. If your birth partner wants to see what’s going on, that’s fine, as long as you feel comfortable with it.
Your doctor will make the cut about 10cm to 20cm along the top of your bikini line, which will have to be shaved for the operation. You may feel some pressure and pulling during the procedure, but no pain6.
Although the actual delivery of your baby only takes around 5 to 10 minutes, the entire length of the procedure is usually around 40–50 minutes5